
Ask DadPad, Infant Feeding, Parenting Advice
Ask DadPad: Breastfeeding – how it works
Posted on 31st August 2020
This is our final blog post on breastfeeding for August, and this time Georgie has looked at the ‘mechanics’ of how breastfeeding works.
In the previous blogs – on colostrum, supporting mum, and breastfeeding myths – we’ve touched upon some of the science and ‘know how’ behind breastfeeding. Today, we’re bringing the detail together in one place because understanding how everything works really does help when you are supporting a breastfeeding mum.
When does breastmilk first start being made, and what’s in it?
Lactation (producing milk) starts at around 20 weeks of pregnancy. Mum-to-be’s breasts will first start to produce a small amount of a thick, sticky substance called colostrum, which will be your baby’s first milk. Despite its appearance, it really does contain all that your baby will need for his first few days of life. Calorie-rich and full of antibodies, colostrum is the perfect first food for your baby’s still-developing digestive system.
In the womb, your baby will have received all that he needed through the umbilical cord, which is attached to the placenta (an organ which attaches baby to mum, through the womb). After your baby is born, and when all the blood has drained from the placenta and back to baby, the placenta will detach from the womb and also be birthed. The action of the placenta detaching from mum triggers a series of hormones which tell mum’s body to start changing the colostrum into mature breastmilk. Mature breastmilk contains everything that your baby will need to grow and develop for the first six months of life, and organisations such as the NHS recommend that breast milk – alongside other foods – should ideally continue to be offered to your baby up until he is at least two years old.
If all is well with mum and baby, they will immediately be offered skin-to-skin after the birth. Skin-to-skin is an important bonding experience that can be done at any time and which has benefits for both you as parents and also your baby [we talked about skin-to-skin in our bonding article]. It is during those first cuddles that baby usually starts to work his way towards a first feed. If, for whatever reason, this doesn’t happen straight away, try not to worry; do, though, make sure that your partner is given the support that she needs to get breastfeeding going as soon as possible.
Regardless of how breastfeeding is started, it is important to remember that frequent breast stimulation helps to activate the milk-making receptors in mum’s breasts and primes them for future milk production.
How is a good supply of milk made and maintained?
Breastmilk is actually made from mum’s blood, and not her stomach contents. Therefore, there is no limit on the kind of food that she can eat when she is breastfeeding.
Hormones from mum’s brain tell her breasts to make, store, monitor and release breast milk. It’s a constant cycle of hormones which occurs during and in between every feed, which means that breastmilk is ready for your baby at any time of the day or night. It is always at the right temperature and it has everything that your baby needs within it. Breasts may change size and firmness throughout the day, depending on how long it has been since baby last fed, but they will never truly be ‘empty’.
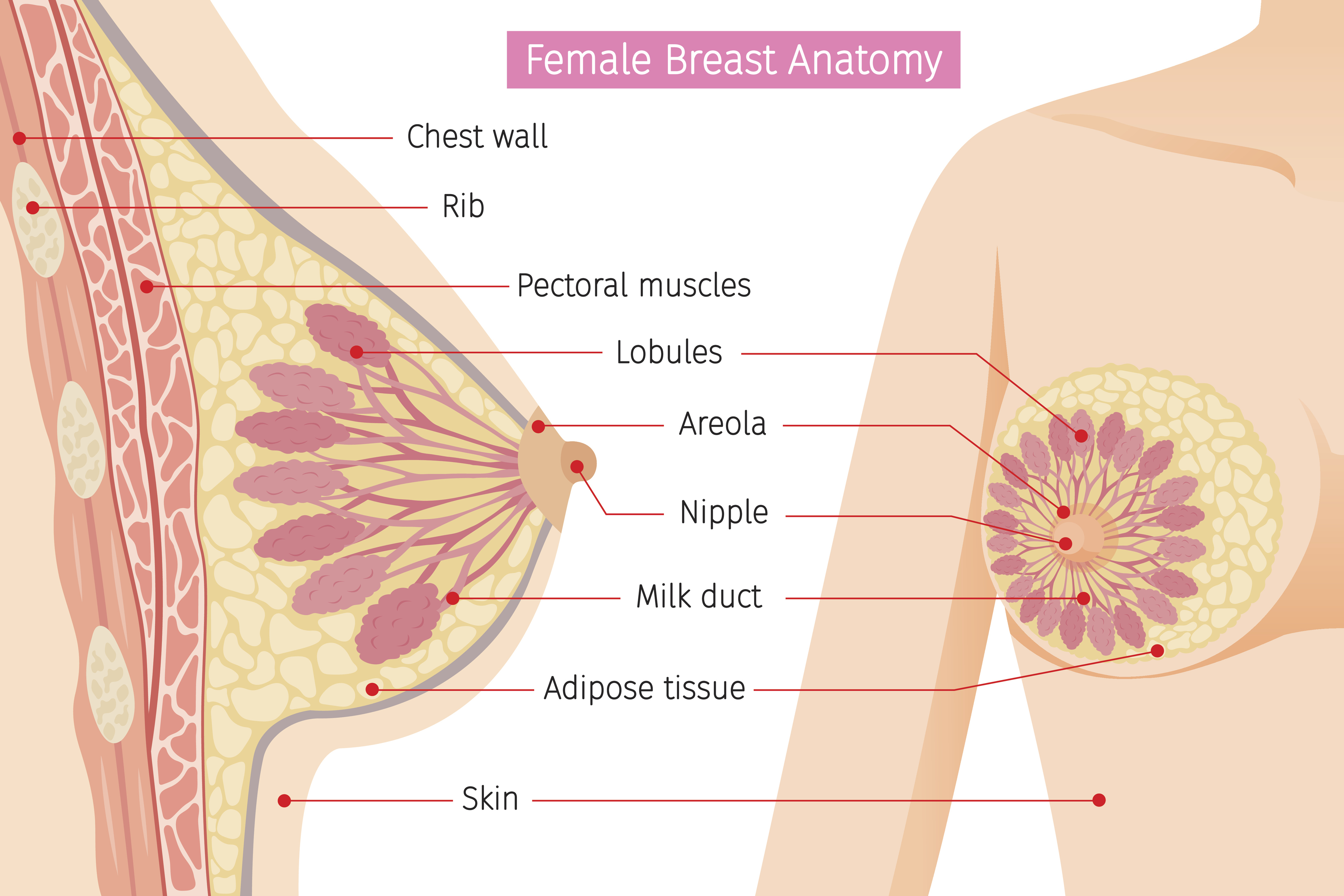
Inside mum’s breasts are lots of little buds (lobules or alveoli) where the milk is made and stored. Tubes (milk ducts) transport the milk from the alveoli to the nipple, and this is all surrounded by muscle and an insulating layer of fatty (adipose) tissue. When your baby starts to feed, mum’s brain sends a message to the tiny muscles in her breasts to contract and squeeze the milk out of the alveoli. As your baby feeds, mum’s hormones also send a signal to start production on the next feed, and when the breasts are full, another hormone will slow down milk production, helping to protect mum from making too much milk. Clever, eh?!
How will I know when my baby is hungry?
Before feeding, you may notice your baby making signs – or cues – that he is ready to be fed. These include:
- Stirring
- Turning his head from side-to-side – sometimes called ‘rooting’
- Poking out his tongue
- Making grumbles and squeaks
- Smacking his lips
- Opening his mouth wide
- Crying
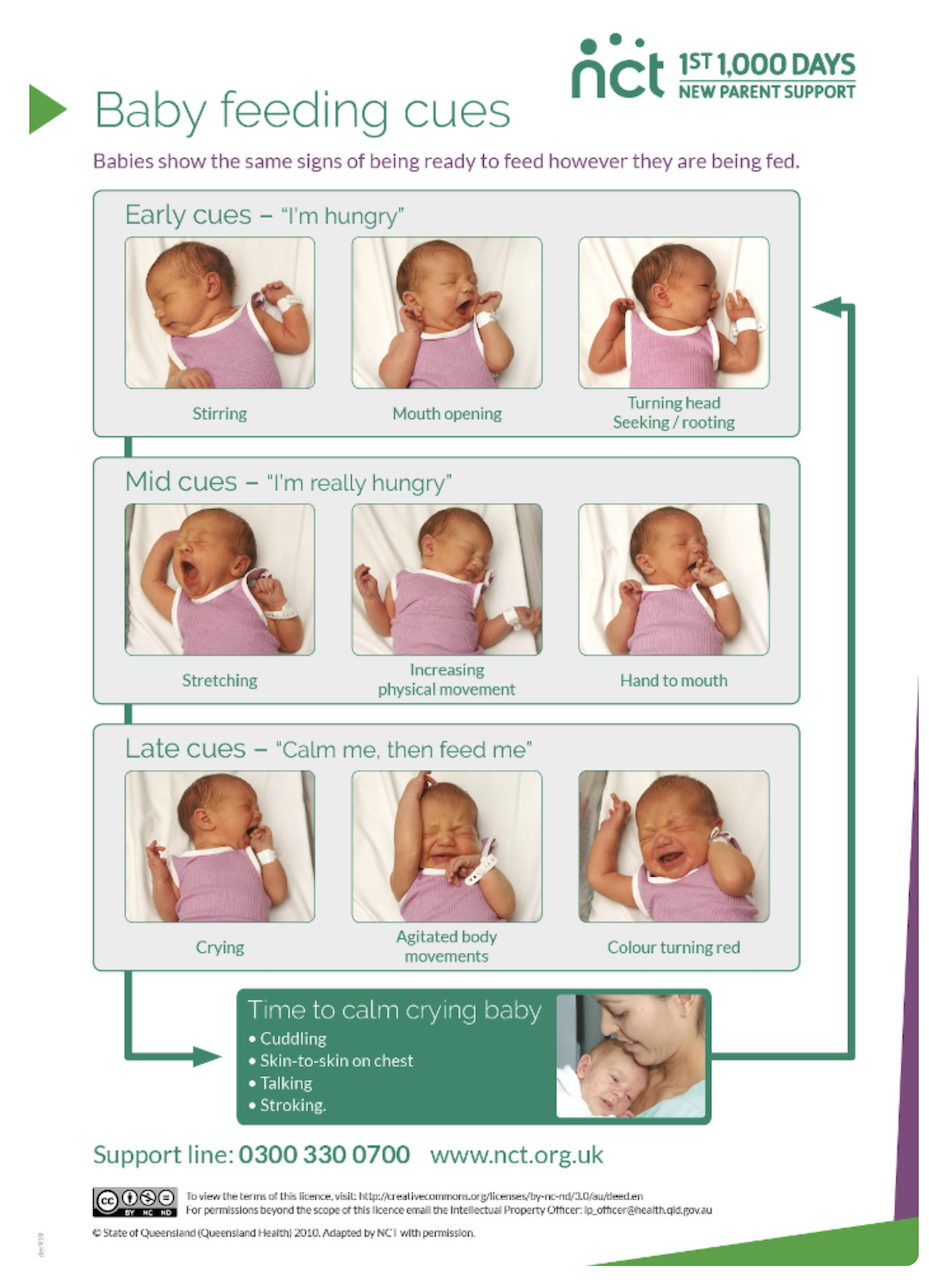
Image from: https://www.nct.org.uk/baby-toddler/feeding/early-days/how-often-should-i-breastfeed-my-baby
These feeding cues are all intended to draw your attention to baby’s needs, and to ensure that he gets fed quickly. Learning to recognise these cues is important in helping to reduce your baby’s potential crying and distress, keeping everyone happy!
What does a good latch look like?
When a baby feeds from the breast, he isn’t actually sucking out the milk, like you would when drinking through a straw. Instead, he’s actually working to stimulate the release of milk and then using his chin and tongue to draw the milk from the breast in a rhythmic action. For this to happen effectively, mum’s nipple and areola (the darker part of her breast, around the nipple) need to be able to go deep into baby’s mouth – this is called ‘the latch’. Making sure that baby gets a deep latch ensures that he can feed properly and prevents potential damage to mum’s breasts.
NB. If mum’s nipples are getting damaged, then this is a sign that baby isn’t positioned or attached quite well enough, and you may want to ask your Midwife or Health Visitor for extra support.

At the start of the feed, you may notice baby kneading the breast tissue with his hands or bobbing his head around. This is all to help stimulate the breasts to release the milk more quickly. As he settles down to feed, you will see the rhythm of the feed change from fast, fluttery sucks to slow long sucks, and back again. This is normal, and means that baby is trying to get the most milk possible from each breast. You may also hear him swallowing and notice him pause from time to time, in order to breathe and have a rest.
What does a good breastfeeding position look like?
There are many different positions in which baby can be fed, and you may need to support your partner to explore which ones are best for her; manoeuvring around after just having had a baby can be challenging. Every position offers its own benefits and mastering a few different positions will help to build mum’s confidence around feeding. Learning to feed lying down is an especially useful skill, to allow mum to rest whilst feeding and also to prevent mum from accidentally dozing off in a potentially unsafe position.
The NHS Start4Life breastfeeding webpage (link below) has good information on three of the most popular breastfeeding positions:
- Cradle hold – or ‘tummy to mummy’
- Mum lying on her side
- Rugby hold – or ‘the clutch’
How will I know if baby is feeding well?
If baby is feeding well, you should be able to see that his lips are pouted out, that he has a good mouthful of breast, his cheeks are rounded and his chin is indented into mum’s breasts. You may even be able to see his little ears wiggle with the motion of his jaw. Although your baby may be very keen to feed, once feeding is under way, both mum and baby should relax into it and be comfortable as the feed continues.
If baby falls asleep during his feed, and you are not sure if he has finished, you can check by winding him or giving him a nappy change and then seeing what happens when the second breast is offered. You will know when your baby is full when he is fully relaxed and unlatches himself from the breast.
Mum will know if breastfeeding is going well for her because:
- She should be comfortable during the feed
- Her nipples should be undamaged
- Her nipples should come out the same shape as when feeding started
- Her nipples should not feel tender or sore between feeds
Initial latching and release of milk can feel intense or uncomfortable, but this sensation should not last for the whole feed. Pain throughout, or between, feeds is a signal to seek further support.
How will I know if baby is getting enough milk?
You will know if your baby is getting enough milk by watching what comes out the other end (!) and by monitoring his growth. In the early days, it’s a good idea to keep a record of how many wet and dirty nappies you see each day and what colour they are; this can be a useful bit of information to have to hand if you are talking to your Midwife, Health Visitor or doctor about your baby’s wellbeing. Plenty of wet and dirty nappies are a sign that your baby is getting enough to eat and drink.

How often does my baby need feeding?
When he is first born, your baby’s tummy will be tiny. Over the coming days and weeks, its capacity will increase. In the early days, then, baby will feed little and often, as the sticky and calorie-rich colostrum provides all the nourishment that your baby needs. As mum’s milk matures, though, the volume of milk produced will increase to match your baby’s needs. Remember that the more mum feeds baby or stimulates her breasts, the more milk that is ‘ordered’ for the next feed.

A newborn baby should feed 8-12 times every 24 hours, and it’s a good idea to keep a record of how often baby is feeding, as this is again useful information to provide to the health professionals supporting your family. It’s also a good idea to note when baby starts feeding, how long the feed lasts and which breast(s) he fed from, so mum knows which breast to offer first at the next feed. A breastfeed baby will feed as much as he needs and doesn’t always feed when he is hungry; breastmilk provides comfort, promotes bonding, calms baby down, relieves pain, as well as quenching thirst and satisfying hunger, too!
When should we seek additional support?
Sometimes, your partner may have doubts about breastfeeding, especially when she is tired or experiencing challenges. You can seek support from your Midwife, Health Visitor, specialist infant feeding team at the hospital, local peer support community, and via the free national support lines. You can even ask Alexa for support now! Further, support can also be accessed privately via: a postnatal support doula with training in supporting breastfeeding; a breastfeeding counsellor; or an International Board Certified Lactation Consultant (IBCLC). We set out information on accessing support in our previous breastfeeding blog.
As the partner in your baby’s care, you will always be welcome when supporting your partner to access further support. Dads play a valuable role in breastfeeding, and the information that any professional shares will be just as important for you to know as your partner. Getting support can be overwhelming for mum, especially if she is trying to remember a number of latch and positioning tips, so going along with her and staying during the support session is a really worthwhile opportunity.

Further information:
We’ve included links to some useful websites and videos which you might like to watch, either on your own or together with baby’s mum, to get more information on all aspects of breastfeeding, starting with this fantastic ‘Introduction to Breastfeeding’ video from the team at Royal Berkshire NHS Foundation Trust:
Breastfeeding Support – Breastfeeding videos – lots of great videos on this page, covering all aspects of position and latch
NHS Start4Life Latching on information – including a really helpful video
NHS Breastfeeding: Positioning and attachment page – again, including a great video
Swansea University – Frequent Feeding Animation – lots of good information on what a ‘normal’ feeding pattern looks like for a breastfed baby
NHS Breastfeeding: Is my baby getting enough milk? – with video
NCT Newborn baby poo in nappies: what to expect – amazing (although quite graphic!) webpage with detailed information on what is ‘normal’ for a health newborn baby to be producing in their nappy
NCT Top five most asked questions about feeding – short but informative video covering: feeding positions, length and frequency of feeds, feeding cues, expressing breastmilk, how do you know if you’re doing it right, and formula feeding

